It usually starts as a faint sensation in the calves — maybe a tingle, maybe a creeping discomfort, hard to describe but impossible to ignore. You shift your legs. The sensation eases for a moment. Then it returns, slightly stronger, demanding movement. By the time you’re lying in bed trying to fall asleep, your legs have a will of their own. Stretching, twitching, kicking. The harder you try to stay still, the more insistent the urge to move becomes. Sleep is somewhere on the other side of this nightly torture, but you can’t get there.
If this resonates, you may have restless legs syndrome (RLS), also known as Willis-Ekbom disease. It affects roughly 7–10 percent of adults in the US and Europe, with women affected nearly twice as often as men. It’s one of the most common causes of sleep onset insomnia in adults. And critically: it’s one of the most treatable causes of insomnia, IF the underlying biology is properly investigated.
In December 2025, the American Academy of Sleep Medicine published new clinical practice guidelines for RLS treatment — the first major update in years. The guidelines reflect significant changes in how the condition is understood and treated, particularly around the role of iron and the problems with long-term dopamine medications. This article explains what RLS is, why it happens, the iron connection that’s often missed, and what the new guidelines mean for getting actual relief.
What Restless Legs Syndrome Actually Is
RLS is a neurological condition characterised by an irresistible urge to move the legs, usually accompanied by uncomfortable sensations — creeping, crawling, tingling, aching, or burning — deep in the legs. The diagnostic criteria, established by the International Restless Legs Syndrome Study Group, require four features:
- An urge to move the legs, usually with uncomfortable sensations
- Symptoms that begin or worsen during periods of rest or inactivity
- Symptoms that are partially or completely relieved by movement
- Symptoms that are worse in the evening or at night
All four must be present. The combination is what distinguishes RLS from other causes of leg discomfort. The evening worsening is the diagnostic giveaway — it tracks the natural circadian decline in dopamine, which is the central clue to what’s actually happening in the brain.
RLS is closely related to a condition called periodic limb movement disorder (PLMD), in which involuntary leg jerks occur during sleep — often without the person knowing. Many people with RLS also have PLMD, and the two conditions share underlying mechanisms. PLMD is detected through sleep studies and can fragment sleep severely even in people who don’t experience the conscious urge-to-move sensation.
Why RLS Wrecks Sleep So Specifically
RLS attacks sleep at exactly the moment of greatest vulnerability — the transition into sleep. Just as your body should be relaxing and your nervous system shifting toward parasympathetic dominance, RLS triggers an urgent need to move. The transition fails. You either lie in bed for hours fighting the sensations, or you get up to walk around, breaking the sleep-bed association entirely.
Even when sleep finally arrives, periodic limb movements can fragment it throughout the night. Sleep studies on RLS patients show:
- Significantly increased sleep onset latency — often 60–90 minutes versus 10–20 in healthy sleepers
- Reduced total sleep time — typically 1–2 hours less than needed
- Fragmented sleep architecture with reduced deep sleep (N3)
- Increased nighttime arousals from periodic limb movements
- Lower sleep efficiency (percentage of time in bed actually asleep)
The cumulative effect is chronic sleep deprivation that compounds the daytime symptoms of the condition itself — fatigue, cognitive impairment, mood changes — creating the feedback loop that makes RLS one of the most quality-of-life-impairing sleep disorders. If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
The Biology: Dopamine, Iron, and the Brain
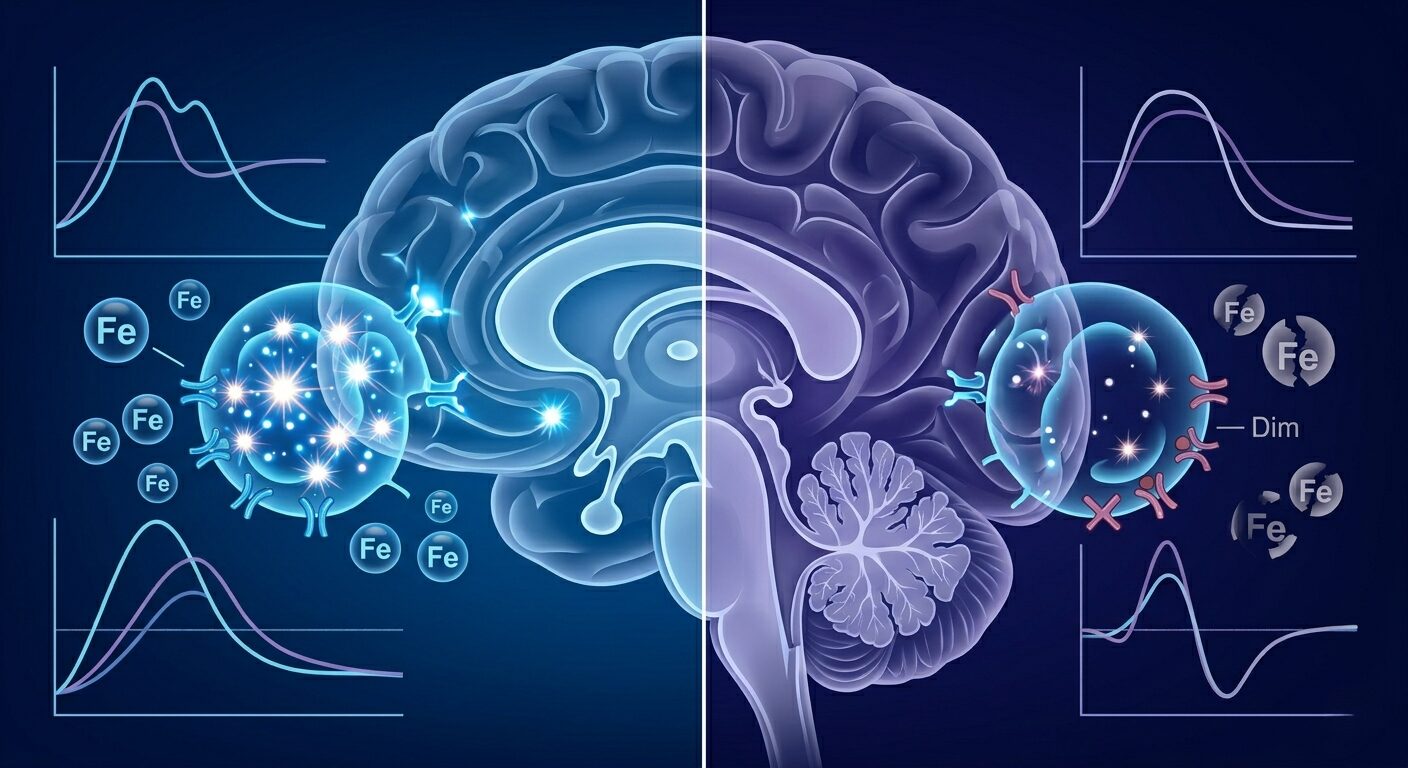
RLS is fundamentally a problem of dopamine signalling in the brain — specifically in the substantia nigra and basal ganglia, the regions responsible for motor control and movement suppression. Healthy dopamine function in these regions does two things relevant to sleep: it suppresses unnecessary movement at rest, and it helps maintain the wake-sleep transition. When dopamine signalling fails, the result is exactly what RLS sufferers describe — movement that won’t suppress, and a sleep transition that won’t complete.
Here’s where iron enters the picture. The enzyme tyrosine hydroxylase — which converts the amino acid tyrosine into the dopamine precursor L-DOPA — requires iron as a cofactor. When brain iron levels are insufficient, dopamine production drops. This isn’t about anaemia or low blood iron in the conventional sense. It’s about specific iron stores in the brain, particularly in dopamine-producing regions.
MRI studies of RLS patients consistently show reduced iron in the substantia nigra, even when serum ferritin appears “normal” by standard lab ranges. This is the central insight that changed how RLS is now understood: it’s often a brain iron deficiency disorder, regardless of what the bloodwork shows.
The Ferritin Gap: Why Your Doctor Said You’re Fine

This is the single most important practical takeaway in this article. Most labs report ferritin as “normal” starting at 12–15 ng/mL. This threshold was established to detect severe iron deficiency anaemia. It is not the threshold required for adequate brain dopamine function in people with RLS.
The International Restless Legs Syndrome Study Group recommends maintaining ferritin above 75 ng/mL for people with RLS. Some sleep specialists target 100+. The new 2025 AASM guidelines explicitly recommend iron supplementation for RLS patients with ferritin below 75 ng/mL, regardless of whether the lab flags the result as abnormal.
The practical implication: a person with RLS and ferritin of 25 ng/mL is told they’re “normal” by their lab, when in reality they’re at one-third of the level their brain needs to function properly. They’re prescribed sleep medications or dopamine agonists when the underlying issue — iron-deficient dopamine production — could often be addressed with iron supplementation. This single disconnect is responsible for an enormous amount of unnecessary suffering.
What the New 2025 AASM Guidelines Recommend
The 2025 American Academy of Sleep Medicine clinical practice guidelines for RLS reflect a significant shift in treatment philosophy. The key recommendations:
Iron is now first-line therapy. Patients with ferritin below 75 ng/mL should receive iron supplementation as the foundation of treatment. Oral iron is recommended for most patients; IV iron is reserved for those who don’t tolerate oral supplementation or fail to raise ferritin levels.
Alpha-2-delta ligands preferred over dopamine agonists. Drugs like gabapentin enacarbil and pregabalin are now preferred over dopamine agonists (pramipexole, ropinirole) for many patients. This is a major change driven by the recognition that long-term dopamine agonist use causes augmentation — a paradoxical worsening of symptoms over time.
Caution against long-term dopamine agonists. Long-term use of dopamine agonists is now strongly cautioned. Many patients who started these medications years ago are now experiencing augmentation — symptoms that have spread to the arms, occur earlier in the day, and become more severe than the original RLS. The new guidelines reflect awareness of this serious adverse outcome.
Lifestyle and trigger management remain important. Iron, magnesium, and B vitamin status are recommended for evaluation. Common triggers — alcohol, caffeine, certain medications including some antidepressants and antihistamines — should be identified and addressed.
Why Iron Levels Are Low in the First Place
Iron deficiency doesn’t happen randomly. The new guidelines emphasise iron supplementation, but the underlying question for any RLS patient should be: why is iron low? Common causes that connect directly to root-cause sleep medicine:
- H. pylori infection — damages the stomach lining and reduces stomach acid, impairing iron absorption. H. pylori is now recognised as a leading cause of iron deficiency that doesn’t respond to oral supplementation.
- Intestinal parasites — directly consume iron and damage the gut wall, creating ongoing iron loss
- Heavy menstrual periods — the most common cause in premenopausal women. Years of menstruation deplete iron stores faster than diet can replace them.
- Gut inflammation and malabsorption — coeliac disease, SIBO, and inflammatory bowel conditions all reduce iron absorption
- Long-term PPI use — reduces stomach acid needed for iron absorption
- Vegetarian and vegan diets — plant-based (non-haem) iron is absorbed 5–10x less efficiently than animal-source (haem) iron
- Chronic blood donation — each donation removes approximately 250 mg of iron, often not fully replaced before the next
- Pregnancy and postpartum — iron stores commonly take 6–12 months to recover after pregnancy, longer in women with multiple pregnancies
This is why oral iron supplementation alone sometimes fails. If H. pylori is impairing absorption, daily iron tablets barely move ferritin levels. The infection has to be treated first to restore the gut’s ability to absorb iron.
What the Research Shows

2025 AASM systematic review: The systematic review accompanying the 2025 guidelines analysed dozens of trials and confirmed iron supplementation produces clinically meaningful improvement in RLS symptoms when ferritin is below 75 ng/mL.
Brain iron deficiency: MRI research consistently shows reduced iron in the substantia nigra and other dopamine-related brain regions in RLS patients, even when serum ferritin appears normal.
Dopamine agonist augmentation: Long-term studies of pramipexole and ropinirole confirm that augmentation occurs in 40–70 percent of patients within 5–10 years of treatment, leading to symptom worsening rather than improvement.
- pylori and iron: Multiple studies confirm H. pylori as a cause of iron deficiency that’s refractory to oral supplementation. Eradication therapy frequently leads to spontaneous improvement in iron status without further supplementation.
Practical Steps for Managing RLS
Test Properly
- Request ferritin specifically, not just haemoglobin or serum iron
- Ask for the actual number, not just whether it’s “normal”
- Target ferritin above 75 ng/mL (some specialists aim for 100+)
- Test for H. pylori if iron is low, particularly if supplementation hasn’t raised levels
- Consider testing magnesium (RBC), B12, and folate — all relevant to RLS
Supplement Strategically
- Iron bisglycinate — best-tolerated form, fewer GI side effects than iron sulphate
- Take with vitamin C (200 mg) to enhance absorption
- Take on an empty stomach if tolerated, or with light food
- Avoid taking with calcium, coffee, tea, or dairy
- Retest ferritin after 3 months to confirm rising levels
Identify and Remove Triggers
- Alcohol — worsens RLS in many patients
- Caffeine, particularly in the afternoon and evening
- Certain antidepressants (SSRIs, SNRIs) and antihistamines (diphenhydramine, doxylamine) — review with prescriber
- Tobacco use
Address Root Causes of Iron Deficiency
- Treat H. pylori or parasites if identified
- Investigate gut absorption issues if iron supplementation isn’t working
- Manage menstrual blood loss with gynaecological evaluation if heavy
- Reconsider long-term PPI use with your prescriber
This article is educational and not medical advice. RLS management benefits from professional guidance, particularly regarding medication choices and high-dose iron supplementation.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
When to Seek Professional Help
Seek professional evaluation if:
- RLS symptoms occur multiple times per week and disrupt sleep
- Your ferritin has never been checked or was checked but not against the 75 ng/mL functional threshold
- You’ve been on dopamine agonists long-term and notice symptoms worsening or spreading
- Iron supplementation hasn’t raised ferritin levels meaningfully — suggesting absorption issues
- RLS coexists with digestive symptoms, fatigue, or other signs of underlying biological issues
Frequently Asked Questions
What causes restless legs syndrome?
RLS is fundamentally a dopamine signalling problem in the brain, often caused by insufficient brain iron levels. Iron is required for dopamine production, and the International RLS Study Group recommends ferritin above 75 ng/mL for adequate function. Other contributing factors include certain medications, alcohol, caffeine, and underlying conditions affecting iron absorption like H. pylori.
What ferritin level do you need for restless legs?
The International RLS Study Group and the 2025 AASM guidelines recommend ferritin above 75 ng/mL for RLS patients. Many conventional labs report 12–15 as “normal” — a threshold designed to detect anaemia, not to support adequate brain dopamine function. Always ask for your specific ferritin number, not just whether it’s flagged as abnormal.
What are the new 2025 RLS treatment guidelines?
The 2025 AASM guidelines emphasise iron supplementation as first-line therapy for ferritin below 75 ng/mL, recommend alpha-2-delta ligands (gabapentin enacarbil, pregabalin) over dopamine agonists for most patients, and caution strongly against long-term dopamine agonist use due to augmentation risk.
Can iron supplements cure restless legs?
For many patients with low ferritin, iron supplementation produces significant improvement and sometimes complete resolution. The key is reaching adequate ferritin levels (above 75 ng/mL) and addressing the underlying cause of iron deficiency — which is often gut-related (H. pylori, parasites, malabsorption).
Why does RLS get worse at night?
RLS symptoms track the natural circadian decline in dopamine levels, which begins in the evening and reaches its lowest point overnight. When dopamine signalling is already impaired (typically by iron deficiency), this evening decline crosses below the threshold needed to suppress motor activity at rest — producing the urge to move that defines RLS.
When to Work With a Sleep Consultant
RLS is one of the most treatable causes of insomnia when the underlying biology is properly investigated. The 2025 guideline shift toward iron-first therapy reflects what root-cause sleep medicine has long emphasised: address the deficiency, treat the underlying cause of the deficiency, and the symptom often resolves. The harder work is identifying why iron is low — which often leads to gut investigation.
Riley Jarvis at The Sleep Consultant works with clients to uncover the root biological causes behind chronic sleep issues and build personalised protocols that address every layer — not just the symptoms.
Book a consultation at TheSleepConsultant.com.






