Candida is a yeast — specifically Candida albicans is the most common species — that lives normally in everyone’s gut, mouth, and on the skin. In small amounts, kept in check by beneficial bacteria and a functioning immune system, it’s harmless. The problem starts when the conditions that suppress candida fail. Beneficial bacteria die off. Immune surveillance drops. Sugar and refined carbohydrates feed an opportunistic species that’s now able to multiply unchecked. Candida transforms from quiet commensal to active overgrowth, and the body starts dealing with consequences far beyond the gut.
Candida overgrowth is one of the most controversial topics in gut health — partly because it’s often discussed in vague, unscientific terms in the wellness world, and partly because conventional medicine has been slow to acknowledge non-invasive intestinal candidiasis as a meaningful clinical entity. But research increasingly supports the connection between gut candida overgrowth and a constellation of systemic symptoms, including persistent fatigue, brain fog, food sensitivities, and yes — chronic insomnia.
This article cuts through the noise. We’ll explore what candida overgrowth actually is, how it disrupts sleep through specific biological mechanisms, the symptoms that suggest it’s happening, and what evidence-based approaches to addressing it look like.
What Candida Overgrowth Actually Is
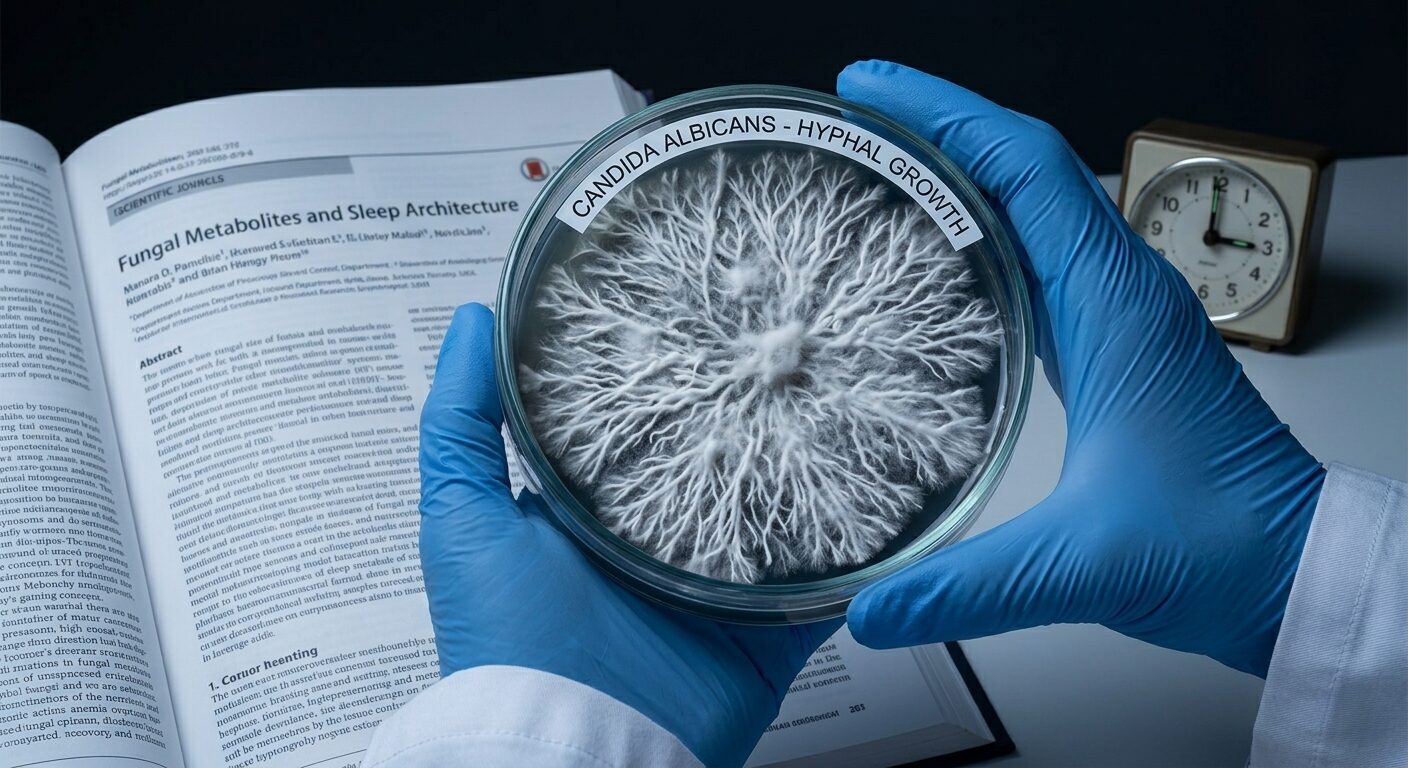
Candida exists in the body in two main forms: yeast and hyphal. The yeast form is the small, oval, single-celled state that lives quietly in mucosal surfaces. The hyphal form is invasive — long, branching filaments that can penetrate tissue, damage cell membranes, and breach barriers like the gut wall. Healthy candida levels are predominantly the yeast form. Overgrowth involves both increased total candida AND a shift toward the hyphal, invasive form.
Several conditions promote this shift. Antibiotic use kills bacteria that normally keep candida suppressed, leaving room for overgrowth. High dietary sugar provides abundant fuel — candida feeds on simple sugars and fermentable carbohydrates. Immune suppression (from medications, chronic stress, or illness) reduces the body’s control. Hormonal changes, particularly elevated oestrogen, can promote candida growth. And gut barrier dysfunction creates an environment where invasive hyphal forms can establish more aggressively.
Importantly, intestinal candida overgrowth is different from the obvious systemic candidiasis seen in immunocompromised patients (which is a serious medical emergency). What we’re discussing here is non-invasive intestinal overgrowth — a more subtle but increasingly recognised pattern that affects otherwise healthy people and produces a wide range of low-grade systemic symptoms over months or years.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
Five Ways Candida Overgrowth Disrupts Sleep
1. Mycotoxin and Metabolite Production
Candida produces a range of byproducts that affect the body systemically when overgrowth is significant. Acetaldehyde — the same compound that produces hangover symptoms after alcohol consumption — is a major candida metabolite. Ethanol is another. Gliotoxin and other mycotoxins can be produced in smaller amounts. These compounds enter circulation through the gut wall and affect liver function, neurological function, and the body’s overall toxic load.
The relevance for sleep: acetaldehyde and ethanol both affect the central nervous system in ways that fragment sleep architecture, mimicking some effects of alcohol consumption even when no alcohol is being consumed. People with significant candida overgrowth sometimes describe waking with hangover-like symptoms despite not drinking. The fungal metabolites are responsible.
2. Blood Sugar Disruption
Candida feeds on sugar. When overgrowth is significant, the yeast actively manipulates host metabolism to maintain fuel access — contributing to blood sugar instability that swings between elevated postprandial spikes and reactive hypoglycaemic crashes. The 3 a.m. blood sugar drop that triggers cortisol and adrenaline release (covered in detail in the blood sugar article) is more common in people with candida overgrowth because the metabolic environment is destabilised.
This is one mechanism by which candida produces the classic 3 a.m. wake-up with racing heart, sweating, and anxiety. The crash isn’t just from poor diet or stress — it’s being driven by a fungal organism actively altering glucose dynamics.
3. Immune Activation and Inflammation
Candida overgrowth triggers chronic immune activation as the body attempts to suppress the population. This produces ongoing low-grade inflammation — elevated cytokines, mast cell activation, increased histamine release. The cytokine elevation specifically reduces deep sleep duration through the same mechanism described in other inflammatory conditions: IL-6, TNF-α, and IL-1β cross the blood-brain barrier and disrupt hypothalamic sleep regulation.
The mast cell activation component is particularly relevant. Candida is a known trigger for mast cell degranulation, which releases histamine. Since histamine is a wake-promoting neurotransmitter, candida-driven histamine release can directly impair sleep onset and maintenance. People with candida overgrowth often have overlapping symptoms of histamine intolerance — congestion, itching, flushing, food sensitivities — alongside their insomnia.
4. Gut Barrier Damage
Hyphal candida can invade the gut wall, damaging tight junctions and increasing intestinal permeability. This contributes to leaky gut, with all its downstream consequences for sleep — endotoxin leakage, systemic inflammation, food sensitivities, and HPA axis activation. The candida-leaky-gut connection means that addressing one without the other rarely produces lasting results. The candida creates the gut damage, the damaged gut allows more systemic effects from candida byproducts, and the cycle reinforces itself.
5. Microbiome Disruption
Candida overgrowth doesn’t exist in isolation — it represents a dysbiotic shift away from microbial diversity and toward fungal dominance. The bacterial species that normally produce GABA, serotonin precursors, and short-chain fatty acids are suppressed. Without these beneficial metabolites, the gut’s contribution to sleep chemistry is compromised. The microbiome shift compounds the direct effects of candida itself.
Symptoms That Suggest Candida Is Affecting Your Sleep
- Insomnia accompanied by digestive symptoms — particularly bloating, gas, and irregular bowels
- Strong sugar and refined carbohydrate cravings, particularly in the evening
- Brain fog that intensifies after eating sugar or carbohydrates
- Persistent fatigue that doesn’t respond to sleep
- Recurrent fungal infections — thrush, vaginal yeast infections, athlete’s foot, fungal nail infections
- White coating on the tongue or persistent bad breath
- Skin issues — eczema, fungal rashes, recurrent acne
- Mood symptoms — anxiety, depression, irritability that arrived alongside the other symptoms
- Hangover-like symptoms in the morning despite no alcohol consumption
- Sleep that worsens after high-sugar or high-carb meals
- History of antibiotic use, oral contraceptive use, or chronic stress
- Histamine intolerance symptoms (congestion, itching, food reactions) alongside insomnia
Who’s at Risk for Candida Overgrowth
Several factors create the conditions for candida overgrowth:
Antibiotic exposure. Antibiotics kill the bacteria that normally keep candida suppressed. Even short courses can produce lasting microbiome changes that allow fungal overgrowth. Multiple antibiotic courses compound the effect significantly.
High-sugar diet. Sugar and refined carbohydrates directly fuel candida. Diets heavy in sweets, processed foods, alcohol (which both feeds candida and disrupts the microbiome), and refined grains promote overgrowth.
Hormonal contraceptives. Oral contraceptive use is associated with increased candida colonisation. The synthetic hormones alter the vaginal and gut environments in ways that favour fungal growth.
Diabetes and insulin resistance. Elevated blood sugar provides ongoing fuel for candida. Diabetics and people with significant insulin resistance have higher rates of fungal overgrowth across multiple body sites.
Immune suppression. Stress, chronic illness, immunosuppressive medications, and chronic infections all reduce the body’s capacity to control candida populations.
Chronic stress. Stress reduces secretory IgA — a key mucosal immune defense — and elevates cortisol in ways that can promote candida overgrowth over time.
What the Research Shows
Candida and inflammation: Research confirms that candida overgrowth triggers immune activation including elevated cytokines, mast cell degranulation, and histamine release. These mediators are documented disruptors of sleep architecture.
Acetaldehyde production: Studies have established that intestinal candida produces acetaldehyde and ethanol as metabolic byproducts. These compounds reach the systemic circulation and affect liver function, central nervous system, and overall toxic load.
Candida and gut barrier: Research demonstrates that hyphal candida can invade and damage the intestinal barrier, contributing to increased permeability and the systemic inflammation that follows.
Antibiotic-candida link: Multiple studies confirm that antibiotic exposure increases the risk of candida overgrowth by suppressing the bacterial competitors that normally maintain fungal balance.
Addressing Candida Overgrowth: An Evidence-Based Approach
Step 1: Confirm Through Testing
Comprehensive stool testing can identify candida overgrowth, including quantification and species identification. PCR-based testing is more sensitive than older culture-based methods. Some practitioners also use organic acids testing, which detects candida metabolic byproducts in urine. Testing helps confirm whether candida is actually involved before committing to lengthy treatment protocols. Many people self-diagnose candida from symptoms alone and end up addressing the wrong issue.
Step 2: Starve the Candida
- Reduce sugar and refined carbohydrate intake substantially — this removes candida’s primary fuel
- Eliminate alcohol — it both feeds candida and damages the gut environment
- Reduce or eliminate fermented sugars — even “natural” sweeteners like honey and maple syrup feed candida significantly
- Be cautious with fermented foods initially — some are well-tolerated, others can worsen symptoms in candida overgrowth
Step 3: Use Antifungal Support
- Botanical antifungals — caprylic acid, oregano oil, berberine, garlic extract, and pau d’arco have evidence for antifungal activity
- For more severe cases, prescription antifungals (nystatin, fluconazole) may be needed under medical supervision
- Saccharomyces boulardii — a beneficial yeast that competes with candida and supports gut barrier function
Step 4: Manage Die-Off
As candida is killed, it releases endotoxins and inflammatory byproducts — producing what’s called a Herxheimer reaction or “die-off.” Symptoms can include headaches, fatigue, brain fog, irritability, and worsening of original symptoms for several days to a few weeks. Supporting elimination during this phase helps reduce symptoms: adequate hydration, gentle binders (activated charcoal, zeolite), liver support, and gentle exercise to support lymphatic drainage.
Step 5: Restore the Microbiome
- Targeted probiotic supplementation — strains with evidence against candida (Lactobacillus rhamnosus GG, Lactobacillus reuteri)
- Diverse plant foods — supports microbial diversity that competes with candida
- Prebiotic fibre — once tolerance is established, supports beneficial bacteria recovery
Step 6: Address Underlying Drivers
Without addressing why candida overgrew in the first place, recurrence is common. This means examining stress patterns, dietary habits, gut barrier function, immune support (vitamin D, zinc), and any underlying conditions that promoted overgrowth. Sustainable resolution requires the conditions for candida overgrowth to be addressed, not just the candida itself eliminated temporarily.
This article is educational and not medical advice. Suspected candida overgrowth benefits significantly from professional evaluation, particularly to confirm diagnosis and guide treatment.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
When to Seek Professional Help
Seek help if:
- Multiple candida symptoms have coexisted with insomnia for months
- History of significant antibiotic use, particularly recent or repeated courses
- Recurrent fungal infections (thrush, vaginal yeast, athlete’s foot) alongside sleep problems
- Strong sugar cravings combined with digestive symptoms and fatigue
- Self-directed candida protocols have produced partial improvement but not resolution
- Symptoms suggest overlap with SIBO, leaky gut, or histamine intolerance — conditions that frequently co-occur with candida
Frequently Asked Questions
Can candida overgrowth cause insomnia?
Yes. Candida overgrowth disrupts sleep through multiple mechanisms: production of acetaldehyde and ethanol that affect the nervous system, blood sugar destabilisation triggering 3 a.m. cortisol surges, immune activation and inflammation that fragment sleep architecture, gut barrier damage, and microbiome disruption that reduces beneficial bacteria producing GABA and serotonin precursors.
What are the symptoms of candida overgrowth?
Common symptoms include digestive issues (bloating, gas), strong sugar cravings, brain fog (especially after carbs), persistent fatigue, recurrent fungal infections, white tongue coating, skin issues (eczema, rashes), mood symptoms, hangover-like mornings without drinking, and overlap with histamine intolerance symptoms (congestion, itching, food sensitivities).
Can candida cause 3 a.m. waking?
Yes — frequently. Candida destabilises blood sugar, increasing the risk of nocturnal hypoglycaemia that triggers cortisol and adrenaline surges in the early morning hours. The classic 3 a.m. wake-up with racing heart, sweating, and anxiety can be driven by candida-induced metabolic dysregulation.
How do I test for candida?
Comprehensive stool testing using PCR technology is the most reliable method, providing both quantification and species identification. Organic acids testing detects candida metabolic byproducts in urine. Many practitioners also use clinical evaluation — symptom patterns, history, and response to treatment — alongside testing to confirm diagnosis.
How long does it take to clear candida?
Treatment typically takes 3–6 months for significant overgrowth, though improvement in sleep and other symptoms often begins within weeks. Successful treatment requires the killing phase (antifungals plus dietary changes), microbiome restoration, gut barrier repair, and addressing the underlying drivers. Without addressing why candida overgrew, recurrence is common.
When to Work With a Sleep Consultant
Candida overgrowth rarely exists in isolation — it typically coexists with leaky gut, SIBO, histamine issues, and microbiome disruption. Successful resolution requires treating candida specifically while also addressing the broader gut environment that allowed it to overgrow. Comprehensive root-cause investigation identifies the full picture so the protocol actually addresses the conditions producing the overgrowth, not just the fungal organism itself.
Riley Jarvis at The Sleep Consultant works with clients to uncover the root biological causes behind chronic sleep issues and build personalised protocols that address every layer — not just the symptoms.
Book a consultation at TheSleepConsultant.com.







