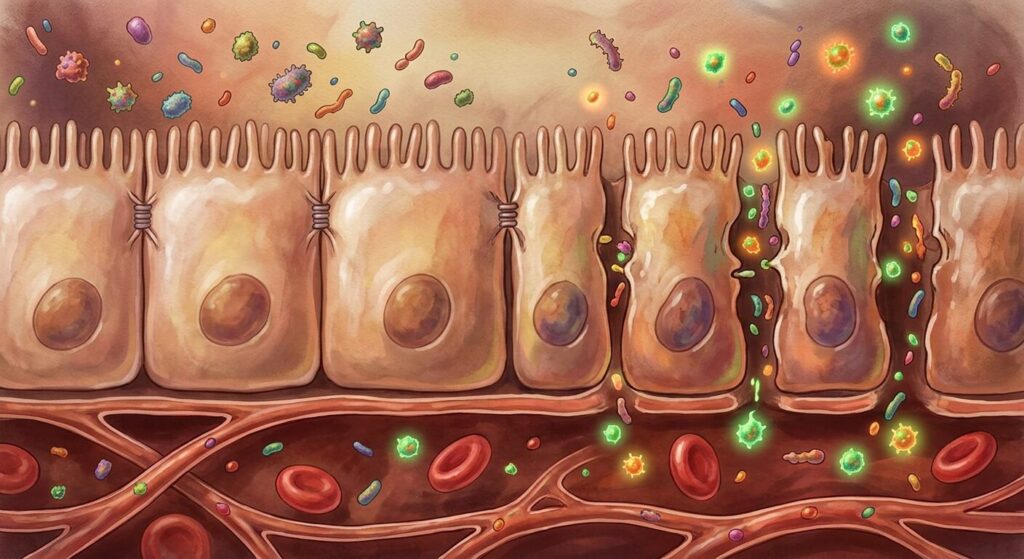
Inside your digestive tract, separating the contents of your gut from the rest of your body, sits a single layer of cells. Just one cell thick. This thin barrier is responsible for selectively allowing nutrients to pass into the bloodstream while keeping bacteria, undigested food particles, and toxins safely contained inside the gut. When this barrier works properly, you don’t notice it. When it fails, the consequences ripple through every system in the body — including your sleep.
Leaky gut — the colloquial name for increased intestinal permeability — is no longer a fringe concept dismissed by mainstream medicine. Researchers now recognise it as a measurable physiological state involved in autoimmune disease, chronic inflammation, food sensitivities, and an expanding list of conditions including chronic insomnia. The connection between leaky gut and sleep isn’t metaphorical. It runs through specific biological mechanisms: systemic inflammation, vagal nerve signalling, serotonin disruption, and immune activation.
This article explains what intestinal permeability actually is, how it disrupts sleep through documented mechanisms, what causes the gut barrier to fail in the first place, and what evidence-based gut healing looks like — the kind that produces sustained sleep improvement, not just temporary symptom relief.
What Leaky Gut Actually Is
The cells lining your small intestine — enterocytes — are connected to each other by structures called tight junctions. These tight junctions act like adjustable gates between cells. They open slightly to allow specific nutrients and water to pass through, then close tightly to maintain the barrier. The tightness of these junctions is regulated by a protein called zonulin. When zonulin levels rise, tight junctions loosen. When zonulin is low, the barrier holds firm.
In a healthy gut, zonulin is released in controlled amounts in response to specific triggers, the barrier briefly opens for legitimate purposes, and then it closes again. In intestinal permeability — leaky gut — zonulin remains chronically elevated, the tight junctions stay loose, and the barrier loses its selective filtering function. Bacteria, bacterial fragments (called endotoxins or LPS), undigested food particles, and inflammatory mediators leak from the gut into the bloodstream where they shouldn’t be.
This isn’t a yes-or-no condition. Permeability exists on a spectrum, and small amounts of “leak” are normal under various physiological circumstances. The problem comes when permeability becomes chronic and significant — when the barrier is essentially broken on an ongoing basis, allowing constant low-grade leakage of substances the immune system was never supposed to encounter. https://thesleepconsultant.com/tired-after-sleeping-8-hours/
Five Mechanisms by Which Leaky Gut Disrupts Sleep
1. Endotoxin Leakage and Systemic Inflammation
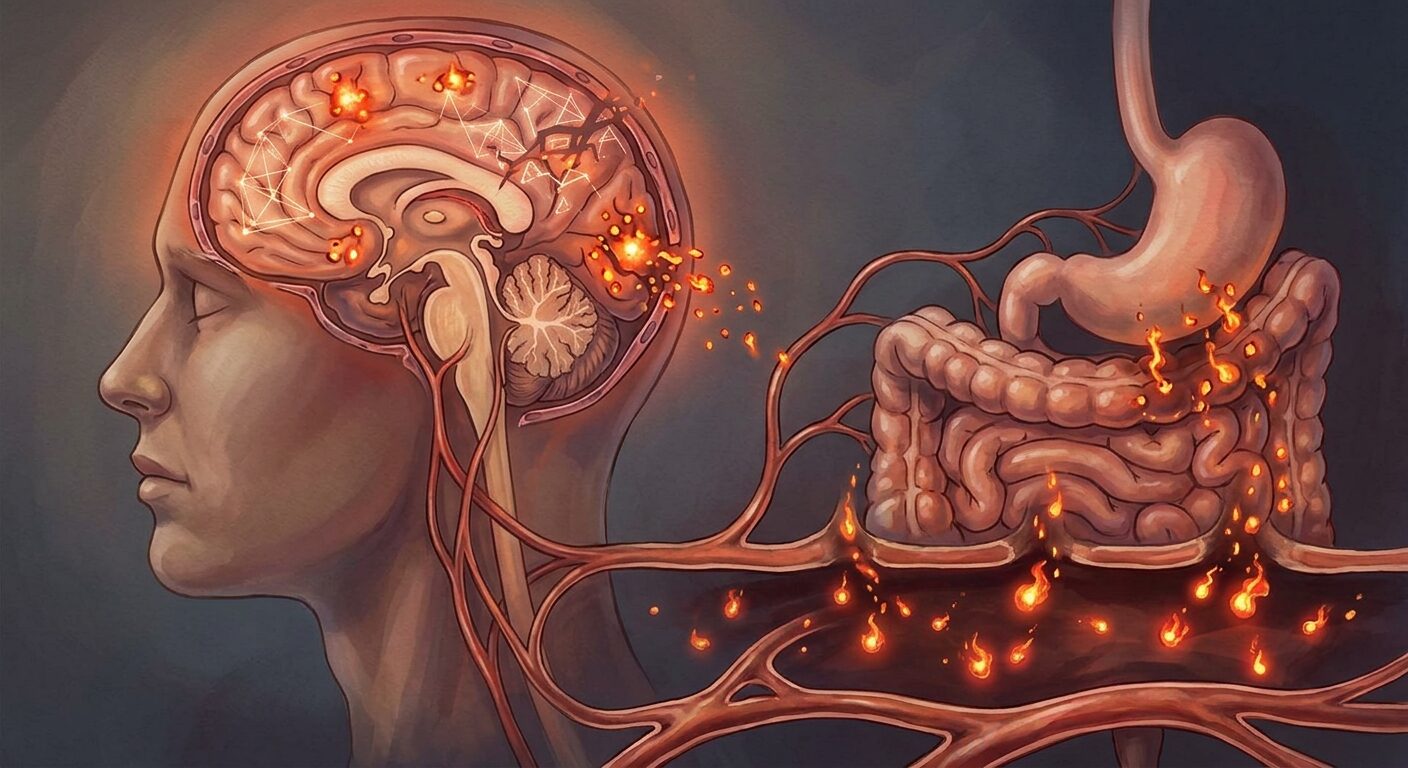
The most direct mechanism. When the gut barrier is compromised, bacterial lipopolysaccharide (LPS) — a component of the outer membrane of gram-negative bacteria — leaks into the bloodstream. The immune system recognises LPS as a sign of bacterial invasion and responds aggressively, releasing inflammatory cytokines including IL-6, TNF-α, and IL-1β. These cytokines circulate throughout the body and cross the blood-brain barrier, where they directly disrupt sleep architecture.
Studies have specifically shown that elevated cytokines reduce deep sleep (N3) duration while preserving lighter sleep stages. People with chronic LPS leakage spend the same time in bed but get less of the restorative deep sleep that physical and immune restoration depend on. The result is the classic pattern of “sleeping enough hours but waking unrefreshed” — because the inflammation is preventing sleep from doing its job.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
2. HPA Axis Activation
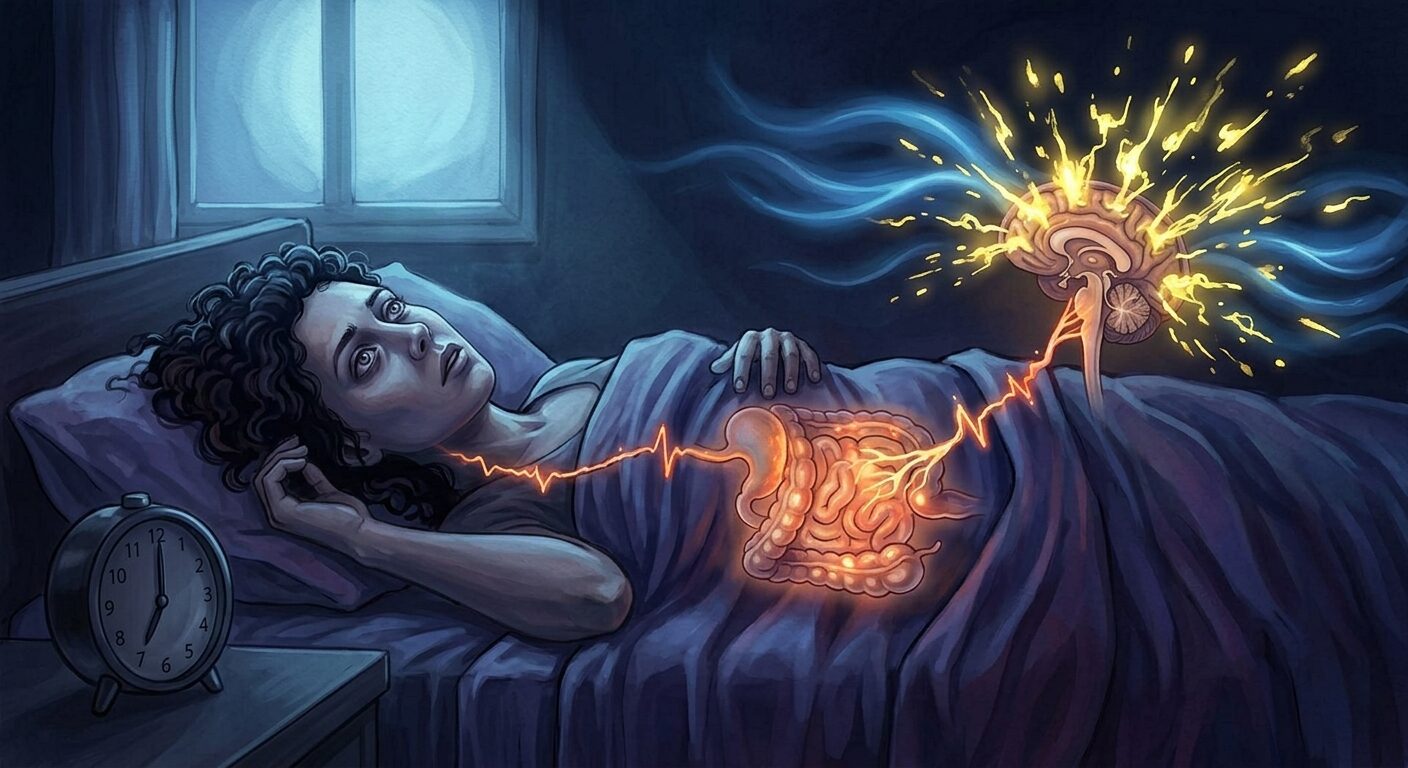
Chronic inflammation from gut barrier compromise activates the hypothalamic-pituitary-adrenal axis as a stress response. The body interprets the persistent inflammatory signals as ongoing threat and responds by elevating cortisol. Over time, this manifests as the cortisol curve disruption that’s central to chronic insomnia: elevated nighttime cortisol blocking deep sleep, flattened curves producing the “wired but tired” pattern, and dysregulated morning cortisol that fails to provide proper waking energy.
This is why people with leaky gut frequently report exactly the cortisol-driven sleep symptoms outlined elsewhere in this library: 3 a.m. waking with racing heart, difficulty falling asleep despite exhaustion, and morning fatigue that no amount of sleep resolves.
3. Vagal Nerve Distress Signalling
The vagus nerve has extensive connections to the gut, including pathways that monitor inflammation and infection. When the gut barrier is compromised and immune activation is occurring, vagal afferent signals carry that information to the brainstem. The brain interprets these signals as evidence of an ongoing threat and responds by maintaining sympathetic nervous system activation.
This mechanism explains why so many people with leaky gut struggle specifically with the transition to sleep. The body remains in low-grade fight-or-flight even when nothing in their environment justifies it. The threat isn’t external — it’s in the gut, signalling persistently up the vagus nerve. Until the gut barrier is restored, the autonomic alarm continues firing.
4. Serotonin and Melatonin Disruption
Approximately 90–95 percent of the body’s serotonin is produced in the gut by enterochromaffin cells. Serotonin is the precursor to melatonin, the primary sleep-initiating hormone. When the gut is inflamed and barrier function is compromised, enterochromaffin cell function suffers, and serotonin production drops. Less serotonin means less melatonin, which means weaker sleep onset signals and shorter sleep maintenance.
The gut barrier compromise also affects tryptophan metabolism. Tryptophan is the amino acid that’s converted to serotonin. When inflammation is high, tryptophan can be diverted away from the serotonin pathway and into the kynurenine pathway, producing metabolites that promote inflammation rather than supporting sleep. This metabolic shift compounds the serotonin deficit and provides another mechanism through which leaky gut undermines sleep at the chemical level.
5. Food Sensitivities and Histamine Release
Once the gut barrier is compromised, food proteins that should remain in the gut can enter the bloodstream where the immune system encounters them. The immune system, having no precedent for these proteins in circulation, may treat them as foreign invaders and develop sensitivities. The result is a slow-developing pattern of food reactions that previously didn’t exist.
These food sensitivities frequently manifest with delayed reactions — hours after eating — that often coincide with bedtime if the trigger food was eaten at dinner. Common reactions include histamine release, mast cell activation, and inflammatory cytokine production, all of which actively interfere with sleep onset and maintenance.
Symptoms That Suggest Leaky Gut Is Affecting Your Sleep
- Insomnia coexisting with digestive symptoms — bloating, irregular bowels, food sensitivities, gas
- Sleep that worsens after specific foods (gluten, dairy, alcohol, processed foods)
- Fatigue disproportionate to sleep deficit — exhaustion that doesn’t match the hours missed
- Brain fog, particularly after meals or in the evening
- Skin issues (rosacea, eczema, acne) alongside sleep problems
- Joint aches or muscle pains without clear cause
- Mood changes — anxiety, depression, irritability — that arrived alongside the sleep changes
- History of antibiotic use, food poisoning, chronic stress, or NSAID use
- Unexplained nutrient deficiencies despite adequate diet
- Autoimmune conditions or family history of autoimmunity
What Causes the Gut Barrier to Fail
Leaky gut doesn’t happen randomly. It results from specific insults to the gut barrier that, when sustained, eventually overwhelm the gut’s capacity to maintain integrity:
Chronic infections. H. pylori damages stomach lining and reduces protective acid. Parasites mechanically damage the gut wall. SIBO produces local inflammation that compromises tight junctions. Each infection is both a cause and an effect of barrier dysfunction.
Dietary triggers. Gluten can stimulate zonulin release in susceptible individuals. Excess sugar feeds dysbiotic bacteria. Alcohol directly damages gut lining. Industrial seed oils promote inflammation. Each individual food matters less than the cumulative dietary pattern.
Medications. NSAIDs (ibuprofen, naproxen) directly damage gut lining with regular use. Antibiotics disrupt the microbiome and can compromise barrier function. Long-term PPI use alters the gut environment in ways that promote permeability.
Chronic stress. Stress directly increases gut permeability through HPA axis effects on tight junctions. This creates a vicious cycle where stress damages the gut, the damaged gut drives inflammation, the inflammation worsens the stress response, and so on.
Environmental toxins. Mold mycotoxins, heavy metals, and various environmental chemicals can damage gut tissue and impair barrier function. This is one mechanism by which mold exposure produces such varied systemic symptoms.
Microbiome imbalance. Dysbiosis — reduced microbial diversity and overgrowth of opportunistic species — alters the gut environment in ways that compromise barrier maintenance. The microbiome and the barrier work together; when one fails, the other follows.
What the Research Shows
Zonulin and disease: Research has established zonulin as a measurable marker of intestinal permeability, with elevated levels documented in coeliac disease, type 1 diabetes, multiple sclerosis, and increasingly in chronic inflammatory and autoimmune conditions.
LPS and inflammation: Studies confirm that lipopolysaccharide leakage from the gut produces systemic inflammation that affects multiple organ systems, including the brain. Elevated LPS markers correlate with depression, anxiety, and cognitive symptoms in human studies.
Cytokines and sleep architecture: Multiple studies confirm that elevated inflammatory cytokines specifically reduce deep sleep duration while preserving lighter stages — the mechanism behind sleeping adequate hours but feeling unrested.
Gut-brain axis review: A 2025 review in Brain Medicine established the microbiota-gut-brain axis as a critical pathway in sleep regulation, providing the framework for understanding how barrier dysfunction translates into neurological and sleep symptoms.
How to Heal Leaky Gut for Better Sleep

Remove the Triggers
- Identify and eliminate foods driving inflammation — a 4-week elimination of gluten, dairy, sugar, alcohol, and processed foods reveals which are problematic for you
- Address chronic infections (H. pylori, parasites, SIBO) through comprehensive testing and targeted treatment
- Reduce NSAID use where possible; discuss long-term PPI use with your prescriber
- Investigate environmental factors — mold exposure assessment if symptoms have a locational pattern
Repair the Barrier
- L-glutamine (5–10 g daily) — the primary fuel source for intestinal epithelial cells. Supports tight junction integrity and barrier repair.
- Zinc carnosine — supports mucosal repair and has direct evidence for improving gut barrier function
- Bone broth — provides collagen, glycine, and proline that support gut tissue repair
- Omega-3 fatty acids — reduce inflammation and support cellular membrane health throughout the gut
- Vitamin D — directly supports tight junction integrity and immune regulation in the gut
Restore the Microbiome
- Dietary diversity — 30+ different plant foods per week supports microbial diversity
- Fermented foods (carefully introduced if histamine issues are present) — yoghurt, kefir, sauerkraut, kimchi
- Targeted probiotic strains with evidence for barrier support — Lactobacillus rhamnosus GG and Bifidobacterium species
- Prebiotic fibre to feed beneficial bacteria — once tolerance is established
Manage Stress
Because chronic stress directly increases gut permeability, stress management is gut healing. Vagal toning practices (extended exhale breathing, cold water on the face, humming) reduce the stress signalling that keeps the gut barrier loose. This is one of the more underappreciated aspects of gut healing — you can’t fully restore the barrier while the nervous system is in chronic activation.
This article is educational and not medical advice. Suspected leaky gut benefits from professional evaluation, particularly to identify and address underlying infections.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
When to Seek Professional Help
Seek help if:
- Insomnia and digestive symptoms have coexisted for more than 3 months
- Multiple food sensitivities have appeared, particularly recently
- You have an autoimmune condition or family history of autoimmunity
- DIY gut healing protocols have helped partially but not fully resolved sleep problems
- Skin issues, joint pain, or mood changes accompany the gut and sleep symptoms
- You suspect underlying infections (H. pylori, parasites, SIBO) but haven’t tested
Frequently Asked Questions
Can leaky gut cause insomnia?
Yes. Leaky gut disrupts sleep through five documented mechanisms: endotoxin (LPS) leakage triggering systemic inflammation that fragments sleep architecture, HPA axis activation elevating cortisol, vagal nerve distress signalling preventing parasympathetic shift, serotonin and melatonin disruption from impaired enterochromaffin cell function, and food sensitivity reactions occurring near bedtime.
What are the symptoms of leaky gut?
Common symptoms include digestive issues (bloating, irregular bowels, food sensitivities), unrefreshing sleep, fatigue, brain fog, skin problems (eczema, acne, rosacea), joint pain, mood changes, and unexplained nutrient deficiencies. Many people also have insomnia or 3 a.m. waking with no obvious cause until the gut connection is investigated.
How do I test for leaky gut?
Zonulin testing measures the protein that regulates tight junction integrity — elevated levels indicate increased permeability. Other markers include LPS antibodies, intestinal permeability assays (lactulose-mannitol test), and comprehensive stool analysis showing inflammation markers. Many practitioners diagnose clinically based on symptom patterns and response to gut healing protocols.
Can healing leaky gut improve sleep?
Yes. Restoring barrier function reduces inflammation, calms vagal distress signalling, supports serotonin and melatonin production, and decreases food sensitivity reactions — all of which directly improve sleep. Many people see meaningful sleep improvement within 4–12 weeks of comprehensive gut healing.
What’s the fastest way to heal leaky gut?
There’s no shortcut, but the most effective approach combines: removing triggers (problematic foods, infections, NSAIDs), repairing the barrier (L-glutamine, zinc carnosine, bone broth, omega-3s), restoring the microbiome (diverse plant foods, targeted probiotics), and managing stress (vagal toning, stress reduction). Underlying infections must be treated for sustained healing.
When to Work With a Sleep Consultant
Leaky gut is one of the most actionable root causes of chronic insomnia, but it rarely exists in isolation. It typically coexists with infections, dysbiosis, food sensitivities, and stress patterns that all need attention. Comprehensive root-cause investigation identifies the full picture so the gut healing protocol actually addresses what’s driving the permeability — not just patches the symptoms.
Riley Jarvis at The Sleep Consultant works with clients to uncover the root biological causes behind chronic sleep issues and build personalised protocols that address every layer — not just the symptoms.
Book a consultation at TheSleepConsultant.com.