You know the feeling. It’s 11 p.m. and you’re wide awake — alert, productive, full of ideas. But six hours ago you could barely keep your eyes open. Morning hits and you feel drugged. By mid-afternoon you’re crashing. Then evening comes and the cycle restarts: tired all day, wired all night.
This isn’t laziness. It’s a timing problem — your internal clock is out of sync with the external world. When that clock drifts far enough, it doesn’t just ruin your sleep. It disrupts metabolism, mood, immunity, and cognition. Everything runs on circadian timing. When the timing breaks, everything downstream breaks with it.
The good news: circadian rhythm disruption is one of the most correctable root causes of chronic sleep problems. But correcting it requires understanding what your body clock is, what knocked it off track, and which signals it needs to recalibrate.
What Is Your Circadian Rhythm?
Your circadian rhythm is a roughly 24-hour internal cycle that governs when you feel awake, when you feel sleepy, when hormones are released, and when virtually every organ system is at peak performance versus recovery mode.
The master clock sits in a tiny brain region called the suprachiasmatic nucleus (SCN), located in the hypothalamus. It takes timing cues primarily from light — specifically blue-spectrum light entering through the eyes — and uses those cues to synchronise the entire body.
But the SCN isn’t the only clock. Nearly every cell contains its own peripheral clock — local timing mechanisms in the liver, gut, muscles, and immune system. Under normal circumstances, the master clock keeps all peripheral clocks aligned. When disruption occurs, these clocks drift out of sync, creating internal misalignment where different systems operate on different schedules.
Think of it like an orchestra without a conductor. Every section is still playing, but no longer together. The result is physiological chaos: sleep problems, digestive issues, mood changes, immune dysfunction, and cognitive impairment — often simultaneously.
Why Circadian Disruption Makes Sleep So Difficult
Sleep is not something your body does simply because you’re tired. It’s something your body does because the circadian system says it’s time. Two independent processes govern sleep onset:
Process S (sleep pressure) is a homeostatic drive that builds the longer you’re awake. Adenosine accumulates in the brain, creating a progressively stronger urge to sleep. This is the system caffeine blocks.
Process C (circadian timing) is the signal from your internal clock that says “now is the window for sleep.” Driven by melatonin release, core body temperature drop, and cortisol suppression — all orchestrated by the SCN.
Healthy sleep requires both processes to align. When your circadian rhythm is disrupted, Process C fires at the wrong time. You’re exhausted — plenty of sleep pressure — but the circadian gate doesn’t open when you want it to. Melatonin arrives late. Temperature doesn’t drop. Cortisol doesn’t suppress. You lie in bed, tired but unable to cross into actual sleep.
This is why circadian disruption produces a specific flavour of insomnia. It’s not anxiety. It’s not pain. It’s your entire physiology not being in “sleep mode” at the time you want to sleep.
Symptoms of Circadian Rhythm Disruption
Circadian disruption doesn’t just affect when you sleep. It affects how you feel, think, digest, and function around the clock.
Sleep Symptoms
- Inability to fall asleep at a socially normal bedtime — you’re alert until midnight, 1 a.m., or later
- Extreme difficulty waking at the desired time — mornings feel physically painful
- Sleep that comes easily at the “wrong” time (e.g., you sleep brilliantly from 3 a.m. to 11 a.m. but can’t sleep from 11 p.m. to 7 a.m.)
- Inconsistent sleep patterns — some nights you crash early, others you’re up until dawn
- Unrefreshing sleep even when duration seems adequate
Daytime Symptoms
- Energy peaks and crashes that follow an abnormal pattern — wired at night, destroyed in the morning
- Brain fog, poor concentration, and slowed decision-making, especially in the morning hours
- Mood disturbance — irritability, anxiety, or depressive feelings that seem to cycle with your energy
- Appetite changes — not hungry in the morning, ravenous at night
- Digestive discomfort — bloating or irregular bowel movements as peripheral gut clocks misalign
Longer-Term Health Signs
- Weight gain, particularly around the midsection, without dietary changes
- Increased susceptibility to illness — the immune system is profoundly circadian-dependent
- Hormonal irregularities — disrupted cortisol curve, altered thyroid function, reproductive hormone shifts
- Blood sugar instability — circadian disruption impairs insulin sensitivity
If your sleep problems feel like a timing issue rather than a falling-asleep-at-all issue — if you can sleep well, just not at the right time — circadian disruption is the most likely culprit. If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
What Actually Happens When Your Body Clock Breaks
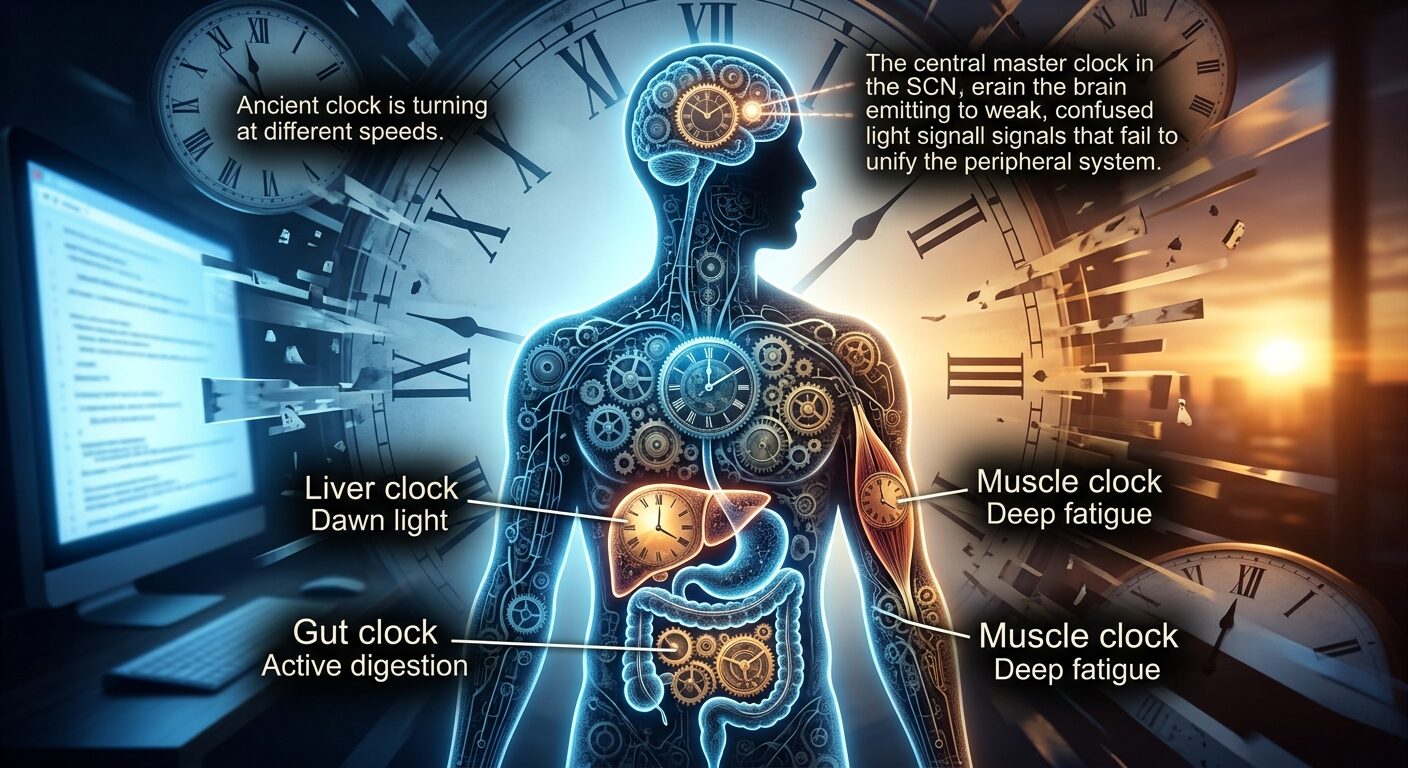
Circadian disruption creates a cascade of hormonal and neurological consequences that extend far beyond “bad sleep.”
Melatonin Timing Shifts
The SCN triggers melatonin release from the pineal gland in response to darkness. When your clock drifts, the melatonin signal arrives too late (delayed phase) or too early (advanced phase). Either way, the chemical “go to sleep” signal no longer aligns with when you need to be sleeping. Supplementing melatonin can help acutely, but doesn’t fix the underlying clock drift.
Cortisol Curve Flattening
A healthy cortisol rhythm peaks sharply within 30–45 minutes of waking and drops steadily through the day, reaching its lowest point during the first half of the night. Circadian disruption flattens this curve: the morning peak is blunted (you can’t wake up) and the evening trough doesn’t fully occur (you can’t wind down). The result is a flat, muddy cortisol profile — under-stimulated by day, over-stimulated at night.
Core Temperature Misalignment
Body temperature follows a circadian cycle, dropping roughly 1–1.5°F before sleep onset. This dip is a critical trigger for falling asleep. When the clock shifts, the drop happens at the wrong time — explaining why some people feel cold and sleepy at 5 p.m. but warm and alert at midnight.
Peripheral Clock Desynchronisation
When the master clock drifts, peripheral clocks in the gut, liver, and immune system desynchronise from each other. Your digestive system expects food at one time; your liver at another. Immune function peaks when it shouldn’t. This internal misalignment is why circadian disruption produces symptoms far beyond sleep — it’s a whole-body timing disorder.
What the Science Says
Circadian disruption and disease: A landmark review in the New England Journal of Medicine established that chronic circadian misalignment is associated with cardiovascular disease, type 2 diabetes, obesity, depression, and impaired immunity. The effects extend far beyond sleep.
Shift work studies: Research on shift workers demonstrates reduced deep sleep, impaired cognition, elevated inflammatory markers, and metabolic dysfunction — even when total sleep hours are maintained. The disruption itself, independent of sleep quantity, causes measurable harm.
Light exposure and clock resetting: Studies in the Journal of Clinical Endocrinology & Metabolism show that properly timed bright light can shift the circadian clock by 1–2 hours per day, making it one of the most powerful non-pharmacological tools for correcting circadian drift.
Meal timing and peripheral clocks: Research in Cell Metabolism demonstrates that meal timing independently entrains peripheral clocks in the liver and gut, even when the master clock receives conflicting signals. Late-night eating can worsen circadian disruption from the periphery inward.
What Causes Circadian Rhythm Disruption?
Your body clock is robust, but it’s not invincible. Several forces can push it out of alignment.
The Obvious Disruptors
- Artificial light at night — screens, LEDs, and overhead lighting suppress melatonin production and delay the circadian sleep signal. This is the single most common cause of circadian drift in modern life.
- Inconsistent sleep and wake times — varying your schedule by more than an hour between weekdays and weekends creates “social jet lag” that prevents the clock from stabilising
- Shift work or frequent time zone changes — forces the body to operate against its biological timing
- Late-night eating — sends timing signals to peripheral clocks that conflict with the master clock’s darkness cue
The Overlooked Disruptors
- Insufficient morning light — your clock needs bright light in the first 30–60 minutes after waking to anchor its timing. Without it, the rhythm drifts later each day.
- Chronic gut infections — H. pylori, parasites, and dysbiosis alter serotonin, melatonin, and inflammatory cytokine production, all of which feed circadian regulation. This is where the gut-sleep connection intersects directly with circadian biology.
- Chronic stress — sustained cortisol elevation flattens the cortisol curve, removing a critical timing anchor
- Nutrient deficiencies — magnesium, B6, and zinc are required for melatonin synthesis. Without them, the clock loses its primary output signal.
Many of these root causes overlap with the gut infections, nutrient depletions, and nervous system issues covered elsewhere on this site. Circadian disruption is rarely the only problem — it’s often the visible surface of a deeper biological issue.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
How to Reset Your Circadian Rhythm Naturally

The circadian clock is designed to be reset by environmental signals called zeitgebers (German for “time givers”). Leveraging these signals correctly is the fastest path back to alignment.
Light: The Master Reset Button
- Get bright outdoor light within 30 minutes of waking — 10–15 minutes of direct sunlight, or 20–30 minutes on overcast days. This is the single most powerful circadian intervention available.
- Dim indoor lighting after sunset. Switch to warm-toned bulbs. Reduce screen brightness or use blue-light filters.
- If you can’t access morning sunlight, a 10,000-lux light therapy box for 20–30 minutes immediately after waking can substitute.
Consistency: Anchor the Clock
- Wake at the same time every day — including weekends. Wake time is the most important single anchor point for circadian stability.
- Set a consistent “lights-down” time 60–90 minutes before your target sleep time to allow melatonin to build
- Resist the urge to sleep in after a bad night. Keeping wake time consistent accelerates recalibration.
Meal Timing: Talk to Your Peripheral Clocks
- Eat your first meal within 1–2 hours of waking to signal “daytime” to the liver and gut
- Finish your last meal at least 3 hours before bed. Late-night eating sends a “daytime” signal to peripheral clocks precisely when they should be winding down.
Temperature: Leverage the Dip
- A warm bath or shower 60–90 minutes before bed accelerates core temperature drop through rapid peripheral heat loss — mimicking the natural circadian temperature dip
- Keep the bedroom cool: 18–19°C (65–67°F) is optimal for most people
Address Underlying Causes
If circadian disruption coexists with digestive symptoms, chronic fatigue, or systemic inflammation, the clock problem may be secondary to a gut infection, nutrient depletion, or HPA axis dysfunction. Light and consistency can reset timing, but if the inputs feeding the clock (serotonin, melatonin precursors, cortisol rhythm) are compromised, the reset won’t hold.
This information is educational and not medical advice. Persistent circadian disruption that doesn’t respond to light and timing interventions warrants professional investigation.
When to Seek Professional Help
Light and timing interventions work for many people. But seek professional support if:
- Your circadian rhythm hasn’t responded to two or more weeks of consistent light exposure and fixed wake time
- Sleep problems coexist with digestive symptoms, chronic fatigue, or unexplained inflammation
- You suspect a gut infection, nutrient deficiency, or hormonal imbalance may be feeding the disruption
- Your circadian shift is severe — you can’t fall asleep before 3–4 a.m. or are waking at 3 a.m. unable to return to sleep
- Mood, cognitive function, or metabolic health are deteriorating alongside the sleep issues
A circadian rhythm that won’t reset despite proper light and timing inputs is often a signal that something upstream is broken — and the clock problem is a symptom, not the root cause.
Frequently Asked Questions
What happens when your circadian rhythm is disrupted?
Circadian disruption causes melatonin to release at the wrong time, cortisol to follow a flattened curve, core temperature to drop out of sync with your sleep window, and peripheral clocks in the gut, liver, and immune system to desynchronise. The result is difficulty falling asleep, poor sleep quality, daytime fatigue, mood changes, digestive issues, impaired immunity, and metabolic dysfunction.
How do you fix a disrupted circadian rhythm?
The most effective interventions are consistent bright light exposure within 30 minutes of waking, a fixed wake time every day (including weekends), dimming lights after sunset, eating meals on a regular schedule, and keeping the bedroom cool. If these don’t work within two to three weeks, an underlying issue like a gut infection or nutrient deficiency may be preventing the clock from resetting.
Can gut health affect your circadian rhythm?
Yes. The gut produces roughly 90–95 percent of the body’s serotonin, which is the precursor to melatonin. Gut infections like H. pylori and parasites can impair serotonin production, alter inflammatory signalling, and deplete nutrients required for melatonin synthesis — all of which directly affect circadian clock function.
How long does it take to reset a circadian rhythm?
With consistent light and timing interventions, most people can shift their circadian clock by 1–2 hours per day. Mild disruption may resolve in one to two weeks. Severe or chronic disruption — especially when compounded by gut health issues or nutrient deficiencies — can take four to eight weeks or longer with professional support.
What is the difference between circadian rhythm disruption and insomnia?
Insomnia is a symptom — difficulty falling or staying asleep. Circadian rhythm disruption is one possible cause. The distinguishing feature is timing: people with circadian disruption can often sleep well at the “wrong” time (e.g., 3 a.m. to 11 a.m.) but struggle at conventional hours. Traditional insomnia involves difficulty sleeping regardless of timing.
When to Work With a Sleep Consultant
If your body clock has drifted and standard fixes aren’t pulling it back, the question isn’t discipline. It’s what’s preventing the clock from responding to normal reset signals — a gut infection disrupting melatonin production, a nutrient deficiency starving the clock, a cortisol pattern so flattened the system has lost its anchor.
Riley Jarvis at The Sleep Consultant specialises in finding what’s underneath a circadian rhythm that won’t reset — investigating gut health, nervous system function, nutrient status, and hormonal patterns to address the root cause, not just the clock.







