Imagine you’re lying in bed. You’re tired. You know you’re tired. Your eyes are heavy. But something inside you won’t let go. There’s a hum of alertness running through your body that feels physical, not mental — a low-grade tension in your chest, a heartbeat that seems a fraction too fast, a sense that your nervous system is running on a frequency that has nothing to do with sleep.
You’re not anxious about anything specific. You’re not worried. Your body just will not switch off.
That experience has a biological name: your nervous system is stuck in sympathetic dominance — fight-or-flight mode — and the nerve responsible for pulling it back into rest-and-repair mode isn’t doing its job. That nerve is the vagus nerve. And when it’s not functioning well, sleep becomes physiologically impossible, no matter how perfect your sleep hygiene is.
What Is the Vagus Nerve?
The vagus nerve is the longest cranial nerve in the body. It originates in the brainstem and wanders (vagus is Latin for “wandering”) through the neck, chest, and abdomen, branching into the heart, lungs, digestive tract, liver, and spleen. It’s the physical backbone of the parasympathetic nervous system — the “rest, digest, and repair” branch that counterbalances the sympathetic “fight or flight” system.
When the vagus nerve fires strongly, your heart rate slows, breathing deepens, digestion activates, inflammation calms, and the body shifts into a state that allows sleep to happen. When vagal tone is weak or the nerve is impaired, the body stays locked in a low-grade alert state — even when there’s no actual threat. You feel safe cognitively, but your physiology doesn’t agree.
The vagus nerve isn’t just relevant to sleep. It’s the master switch between “on” and “off” for the entire autonomic nervous system. And sleep is the ultimate “off” state — the deepest expression of parasympathetic dominance your body achieves in a 24-hour cycle. If the vagus nerve can’t get you there, nothing else will.
Why Vagus Nerve Dysfunction Wrecks Sleep
Sleep onset isn’t a passive event. It’s an active transition — your nervous system must actively shift from sympathetic tone to parasympathetic tone. The vagus nerve orchestrates this shift. When vagal function is impaired, the transition stalls.
Think of it like a car that can accelerate but can’t brake. The engine (sympathetic system) runs fine. But without brakes (vagus nerve), you can’t slow down. You can’t stop. You can’t park. And sleep is parking.
This is why vagus nerve-related insomnia feels so specific. It’s not racing thoughts keeping you awake — it’s a physical inability to downshift. People often describe it as feeling “wired in the body” even when the mind is calm. That’s sympathetic tone that the vagus nerve can’t override.
Signs That Your Vagus Nerve Is Affecting Your Sleep
Vagus nerve dysfunction doesn’t show up in a typical sleep report. It shows up in how your body feels around sleep — and in a constellation of daytime symptoms that point to autonomic imbalance.
At Night
-
Physical tension or restlessness at bedtime that isn’t relieved by relaxation techniques
-
Heart rate that feels elevated or irregular when lying down
-
Shallow breathing that you have to consciously override
-
A feeling of internal “buzzing” or alertness that’s physical, not mental
-
Difficulty transitioning from wakefulness to sleep — you hover at the threshold without crossing
-
Waking in the night with a jolt or a spike of adrenaline
During the Day
-
Digestive sluggishness — bloating, constipation, or slow motility (the vagus nerve drives gut movement)
-
A weak or absent gag reflex (the vagus nerve controls it)
-
Difficulty taking deep, satisfying breaths
-
Chronic low-grade anxiety that feels more physical than emotional
-
Heart rate variability (HRV) that’s consistently low on a wearable tracker
-
Feeling “stuck in overdrive” — unable to fully relax even in safe, calm environments
The pattern to watch for: sleep difficulty that feels like a body problem rather than a mind problem, combined with signs of poor parasympathetic function during the day. This is the vagus nerve signature.
How the Vagus Nerve Controls the Sleep Transition
The vagus nerve influences sleep through four primary mechanisms, each operating through a different branch of the autonomic and immune systems.
1. Autonomic Switching
The transition from wakefulness to sleep requires a shift in autonomic balance — sympathetic tone must decrease while parasympathetic tone increases. The vagus nerve is the primary driver of this parasympathetic surge. When vagal tone is high, the transition is smooth: heart rate drops, blood pressure falls, breathing slows, and the body enters a physiological state compatible with sleep. When vagal tone is low, the sympathetic system remains dominant and the transition either fails or is incomplete — leading to light, fragmented sleep.
2. Heart Rate Variability and Sleep Quality
Heart rate variability (HRV) — the natural variation in time between heartbeats — is a direct measure of vagal tone. Higher HRV indicates stronger vagal input and better autonomic flexibility. Research consistently shows that higher HRV is associated with better sleep quality, more deep sleep, and easier sleep onset. Low HRV signals a nervous system stuck in sympathetic mode, and it’s one of the most reliable biomarkers for predicting poor sleep.
3. The Gut-Brain Axis
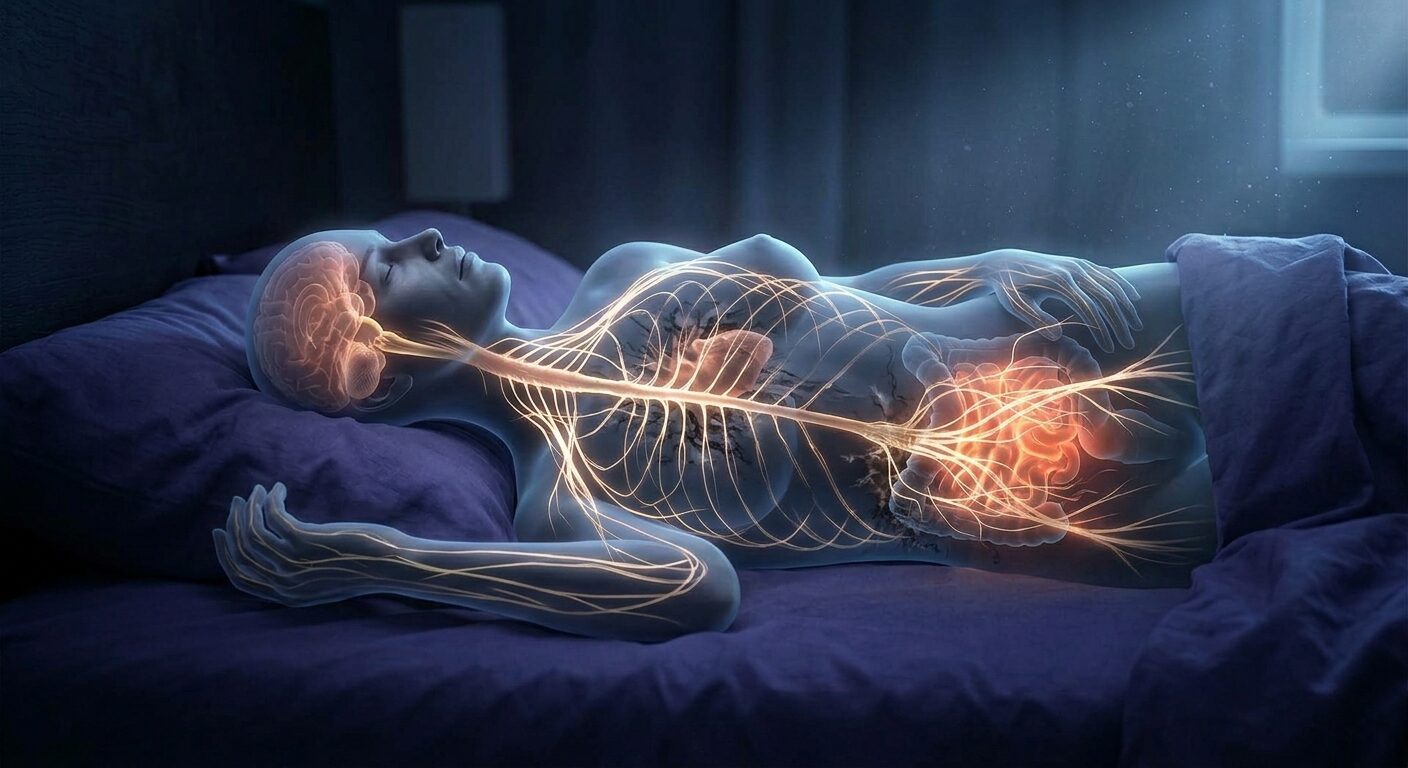
The vagus nerve is the primary communication highway between the gut and the brain. Roughly 80 percent of vagal fibres are afferent — they carry information from the gut to the brain, not the other way around. This means the condition of your gut directly influences how your brain regulates sleep, mood, and stress.
When the gut is inflamed — from H. pylori, parasites, dysbiosis, or intestinal permeability — the vagus nerve transmits distress signals to the brain. These signals activate the stress response, suppress parasympathetic tone, and impair the brain’s ability to initiate and maintain sleep. This is the mechanism that connects gut infections to insomnia, and the vagus nerve is the wire it travels on.
4. Inflammatory Regulation
The vagus nerve operates the “cholinergic anti-inflammatory pathway” — a mechanism through which vagal signalling suppresses the production of pro-inflammatory cytokines. When vagal tone is high, systemic inflammation stays low. When vagal tone drops, inflammation rises unchecked. Since elevated cytokines (IL-1, IL-6, TNF-α) directly impair sleep architecture, weak vagal function creates a double hit: the nervous system can’t relax, and the inflammatory environment actively disrupts whatever sleep does occur.
What the Research Shows
HRV and sleep quality: A meta-analysis in Psychophysiology confirmed that higher resting HRV — indicating stronger vagal tone — is significantly associated with better sleep quality, shorter sleep onset latency, and more time spent in deep sleep.
Vagus nerve stimulation (VNS): Clinical studies on transcutaneous vagus nerve stimulation have demonstrated improvements in sleep quality, reductions in insomnia severity, and increased parasympathetic tone during sleep. A 2021 study in the Journal of Clinical Sleep Medicine found that auricular VNS improved both subjective and objective sleep measures in chronic insomnia patients.
The cholinergic anti-inflammatory pathway: Research published in Nature has established that vagus nerve signalling directly suppresses inflammatory cytokine production via the cholinergic pathway. This mechanism positions vagal tone as a key regulator of the inflammatory environment that determines sleep quality.
Gut inflammation and vagal signalling: Studies in Neurogastroenterology & Motility have shown that intestinal inflammation impairs vagal afferent signalling, creating a feedback loop: gut infection → vagal dysfunction → increased stress response → worsened gut inflammation → further vagal impairment.
What Damages Vagus Nerve Function
Vagal tone isn’t fixed. It’s dynamic and responsive to both damage and training. Understanding what impairs it explains why your nervous system may be stuck.
-
Chronic stress — sustained sympathetic activation literally down-regulates vagal output over time. The longer the stress persists, the weaker the vagal brake becomes.
-
Gut infections — H. pylori, parasites, and SIBO inflame the intestinal wall where vagal nerve endings are densely concentrated. This inflammation directly impairs vagal signalling.
-
Physical trauma — whiplash, neck injuries, and surgical procedures involving the throat or abdomen can physically damage vagal nerve branches
-
Chronic inflammation from any source — autoimmune conditions, mould exposure, metabolic dysfunction — suppresses vagal activity through the same cytokine pathways the vagus nerve is supposed to regulate
-
Sedentary lifestyle — physical activity is one of the most reliable ways to strengthen vagal tone. Its absence allows tone to decay.
-
Poor breathing patterns — chronic shallow, chest-dominant breathing fails to stimulate the vagus nerve branches in the diaphragm, reducing parasympathetic input throughout the day
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
How to Strengthen Vagal Tone and Restore Sleep
The vagus nerve is trainable. Unlike many biological systems, vagal tone responds rapidly and measurably to targeted interventions. Most people notice changes in HRV and sleep quality within days to weeks.
Breathing: The Most Direct Access Point

The vagus nerve has branches embedded in the diaphragm. Slow diaphragmatic breathing with extended exhales directly stimulates vagal output, shifting the autonomic balance toward parasympathetic.
-
Aim for 5–6 breaths per minute — roughly 4–5 seconds in, 6–8 seconds out
-
The exhale is what matters most. A longer exhale activates the vagal brake via the baroreceptor reflex.
-
Practice for 5–10 minutes before bed as a pre-sleep transition tool. Consistency is more important than duration.
Cold Exposure: The Dive Reflex
Splashing cold water on the face — or immersing the face in cold water for 15–30 seconds — triggers the mammalian dive reflex: an involuntary vagal response that slows heart rate and shifts autonomic tone toward parasympathetic within seconds. This is one of the fastest vagal activation techniques available.
Vocal Activation: Humming, Gargling, Chanting
The vagus nerve innervates the muscles at the back of the throat. Vigorous gargling (with enough force to challenge the muscles), sustained humming, and resonant chanting all stimulate these branches. Brief daily practice strengthens vagal tone over time.
Physical Activity
Aerobic exercise is one of the most evidence-backed ways to increase vagal tone. Even moderate activity — brisk walking, swimming, cycling — improves HRV within weeks. The effect is both acute (single sessions temporarily boost vagal tone) and chronic (regular exercise permanently elevates baseline HRV).
Address the Gut
If a gut infection is inflaming the vagal nerve endings in the intestinal wall, no amount of breathing exercises will fully restore vagal function. The inflammation must be resolved. Testing for H. pylori, parasites, and gut dysbiosis — and treating what’s found — removes the source of the vagal impairment.
This is why vagus nerve exercises sometimes help partially but never completely resolve the insomnia. They strengthen the nerve’s output, but if the nerve is being actively damaged by an ongoing gut infection, the improvement has a ceiling.
This information is educational and not medical advice. Persistent nervous system dysregulation warrants professional investigation.
When to Seek Professional Help
Consider professional support if:
-
Your insomnia feels physical rather than mental — your body won’t relax even when your mind is calm
-
Breathing exercises and relaxation techniques help partially but can’t fully resolve the problem
-
Your HRV is consistently low and not responding to exercise or stress management
-
You have concurrent gut symptoms suggesting an infection that may be impairing vagal function
-
You’ve experienced a neck injury, surgery, or physical trauma that may have affected the vagus nerve
-
Digestive sluggishness, chronic inflammation, or autonomic symptoms accompany the sleep problems
When the vagus nerve is impaired by an active gut infection or chronic inflammation, behavioural interventions alone won’t be enough. The source of the impairment needs to be identified and resolved.
Frequently Asked Questions
Can the vagus nerve cause insomnia?
Yes. When vagus nerve function is impaired (low vagal tone), the body struggles to shift from sympathetic (fight-or-flight) to parasympathetic (rest-and-repair) mode. This makes the transition into sleep physiologically difficult, causing difficulty falling asleep, light fragmented sleep, and nighttime waking with physical arousal symptoms like elevated heart rate.
How do you stimulate the vagus nerve for sleep?
The most effective techniques include slow diaphragmatic breathing with extended exhales (5–6 breaths per minute), cold water on the face to trigger the dive reflex, humming or gargling to activate vagal branches in the throat, and regular aerobic exercise to raise baseline vagal tone. Practice these consistently, particularly in the 30–60 minutes before bed.
Can gut problems affect the vagus nerve?
Yes. The vagus nerve has extensive branches in the intestinal wall. Gut infections like H. pylori and parasites inflame these branches, impairing vagal signalling and creating a feedback loop between gut inflammation and nervous system dysregulation. This is one of the key pathways connecting gut health to insomnia.
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
What does low vagal tone feel like?
Low vagal tone often manifests as a physical inability to relax — an internal buzzing or tension even in calm environments. Other signs include elevated resting heart rate, low heart rate variability, digestive sluggishness, shallow breathing, chronic low-grade anxiety that feels more physical than emotional, and difficulty transitioning into sleep.
How long does it take to improve vagal tone?
Most people see measurable improvements in HRV and sleep quality within 1–3 weeks of consistent vagal toning practices (breathing exercises, cold exposure, physical activity). However, if an underlying gut infection or chronic inflammation is impairing the vagus nerve, full restoration requires addressing the root cause alongside the exercises.
When to Work With a Sleep Consultant
If your body won’t switch off at night — if the problem feels like it lives in your nervous system rather than your thoughts — you’re dealing with something deeper than sleep hygiene can fix. The vagus nerve is trainable, but when it’s being actively impaired by a gut infection, chronic inflammation, or unresolved physical stress, training alone has a ceiling.
Riley Jarvis at The Sleep Consultant specialises in identifying the root causes of nervous system dysregulation — gut infections, inflammatory drivers, nutrient deficiencies, and HPA axis dysfunction — and building personalised protocols that restore vagal function and sleep from the ground up.
If your nervous system is stuck in overdrive and nothing has been able to turn it off, book a consultation at TheSleepConsultant.com.