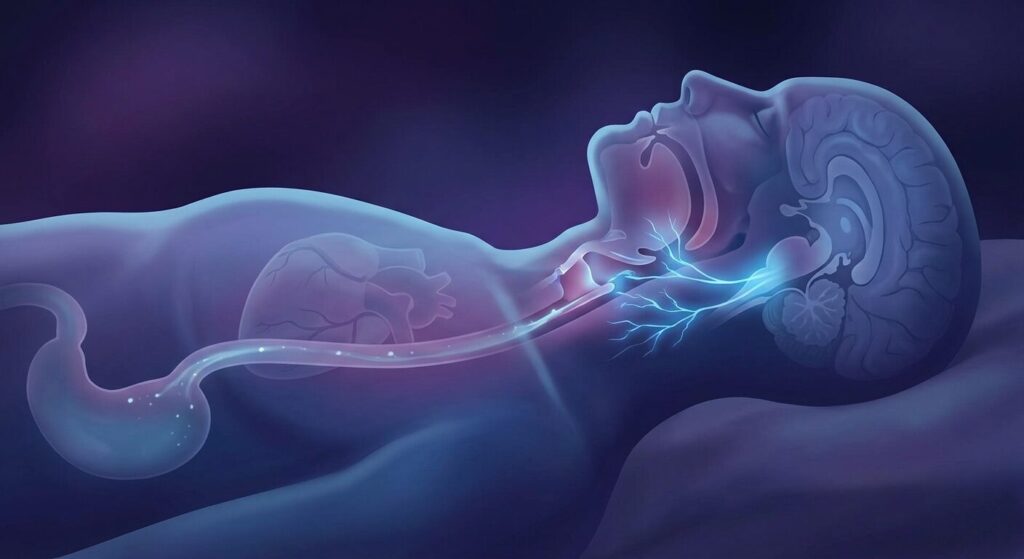
When most people think of acid reflux, they picture heartburn — that unmistakable burning behind the breastbone after a heavy meal. If they don’t get heartburn, they assume reflux isn’t their problem. But there’s a form of reflux that never produces the classic burn, never announces itself with chest pain, and can silently fragment your sleep for months or years without anyone making the connection.
It’s called laryngopharyngeal reflux (LPR), or “silent reflux.” Acid travels up from the stomach, past the oesophagus, and reaches the throat and airway. The throat tissue has different pain receptors than the oesophagus, so you don’t feel the burning. But the acid still triggers vagal nerve irritation, micro-awakenings, coughing, and autonomic disruption — all happening during the night, all without producing a symptom you’d recognise as reflux.
If you wake in the early-morning hours with throat irritation, a need to clear your throat, a dry cough, or unexplained alertness — and these symptoms worsen after eating late or drinking alcohol — silent reflux deserves investigation as a root cause of your sleep disruption. It’s one of the most commonly missed connections in sleep medicine.
How Acid Reflux Disrupts Sleep — Even Without Heartburn
Stomach acid production follows its own circadian rhythm, with output peaking in the late evening and early morning hours. During the day, gravity helps keep stomach contents below the oesophageal sphincter. But when you lie flat at night, that gravitational advantage disappears. If the lower oesophageal sphincter is weakened — by H. pylori infection, hiatal hernia, chronic inflammation, or simply eating too close to bedtime — acid refluxes upward during peak production hours.
The oesophagus and throat are heavily innervated by the vagus nerve. When acid contacts these vagal nerve endings, it triggers a cascade of responses:
-
Micro-awakenings — brief cortical arousals (lasting seconds) that reset sleep cycles without reaching full consciousness. You don’t remember waking, but polysomnography shows dozens of these events per night.
-
Autonomic shifts — vagal irritation pushes the nervous system toward sympathetic activation, elevating heart rate and disrupting the parasympathetic dominance that sleep depends on
-
Reflexive swallowing and coughing — the body’s attempt to clear acid from the throat, often registered only as a vague sense of throat discomfort in the morning
-
Bronchospasm — in severe cases, acid reaching the airway can trigger constriction, causing coughing fits or breathing difficulty during sleep
Studies using overnight pH monitoring combined with polysomnography confirm that reflux events cluster in the 1–4 a.m. window — precisely when sleep architecture is lightest and most vulnerable. A single reflux event can shift the brain from deep sleep to light sleep, and multiple events across the night can reduce total deep sleep by 30–50 percent without the sleeper ever knowing reflux was the cause. If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
Symptoms That Suggest Silent Reflux Is Disrupting Your Sleep

-
Waking between 1 and 4 a.m. without a clear cause, sometimes with a jolt of alertness or a vague sense of discomfort
-
Morning hoarseness, sore throat, or a persistent need to clear the throat upon waking
-
A sour or metallic taste in the mouth first thing in the morning
-
A chronic dry cough that’s worse at night or upon waking — often misdiagnosed as allergies or post-nasal drip
-
Throat mucus or a “lump in the throat” sensation (globus) that doesn’t respond to allergy treatment
-
Sleep disruption that noticeably worsens after eating late, eating spicy or fatty food, or drinking alcohol
-
Symptoms that improve when sleeping on the left side or with the head elevated
-
Dental erosion on the back surfaces of teeth — a sign acid has been reaching the mouth during sleep
The critical distinction that gets missed: classic GERD announces itself with chest burning. Silent reflux announces itself with sleep disruption, morning throat symptoms, and chronic cough. Many people with LPR have been investigated for insomnia, anxiety, allergies, or asthma without anyone looking at their oesophagus. The reflux connection only becomes visible when you look at the pattern: symptoms that are worse lying flat, worse after eating late, worse after alcohol, and better with left-side sleeping and head elevation.
The Biological Mechanisms: Why the Vagus Nerve Makes This a Sleep Problem
The reason silent reflux disrupts sleep so profoundly — even without causing pain — comes down to the vagus nerve. The vagus nerve runs from the brainstem through the neck, chest, and abdomen, and has extensive branches in the oesophagus and throat. When acid contacts these branches, the vagus sends afferent signals to the brainstem that trigger arousal responses, autonomic shifts, and protective reflexes.
This is the same nerve that orchestrates the shift from sympathetic to parasympathetic dominance during sleep. When it’s being irritated by acid, it can’t perform its sleep-maintenance role effectively. The body gets caught between two competing vagal demands: the calming signals needed for sleep and the alarm signals triggered by acid in the wrong place. Sleep loses.
Over time, chronic nocturnal reflux can impair overall vagal tone. Lower vagal tone means weaker parasympathetic function, which means lighter sleep, lower HRV, and reduced capacity for autonomic recovery during sleep. The reflux doesn’t just fragment individual nights — it progressively weakens the nervous system’s ability to produce restorative sleep at all.
The H. Pylori Connection: The Infection Behind the Reflux
H. pylori is one of the most common underlying causes of both classic GERD and silent reflux. The bacterium damages the stomach lining, alters acid production patterns (sometimes increasing acid in the antrum, sometimes reducing it overall in ways that paradoxically worsen reflux), and weakens the protective mechanisms that keep acid where it belongs. It also creates chronic inflammation that disrupts the HPA axis, depletes nutrients needed for sleep, and impairs the gut’s serotonin production.
This is why acid reflux and insomnia so often appear together as part of a larger pattern. H. pylori doesn’t just cause reflux. It causes reflux AND cortisol dysregulation AND nutrient depletion AND serotonin reduction AND vagal impairment — hitting sleep from five directions simultaneously. Treating the reflux symptom (with PPIs or antacids) without investigating the underlying infection produces temporary relief at best. Treating the infection often resolves the reflux, the insomnia, and the other symptoms that came with it.
What the Research Shows

Reflux and sleep architecture: Research using simultaneous pH monitoring and polysomnography confirms that nocturnal acid reflux events cause measurable micro-awakenings and shifts from deep to light sleep, even when the sleeper doesn’t report conscious waking. A single reflux event can disrupt an entire sleep cycle.
Silent reflux prevalence: Studies estimate that up to 50 percent of patients with chronic throat symptoms (hoarseness, cough, throat clearing) have laryngopharyngeal reflux rather than allergies or infection. The condition is dramatically underdiagnosed because patients and doctors don’t associate these symptoms with acid.
H. pylori and reflux: Research confirms that H. pylori alters gastric acid dynamics and that eradication therapy improves reflux symptoms in a significant subset of patients, particularly those with antral-predominant infection.
Position and reflux: Studies in the American Journal of Gastroenterology consistently show that left lateral decubitus position reduces oesophageal acid exposure by 70–80 percent compared to right-side and supine sleeping.
How to Address Reflux-Related Sleep Disruption
Positional Strategies
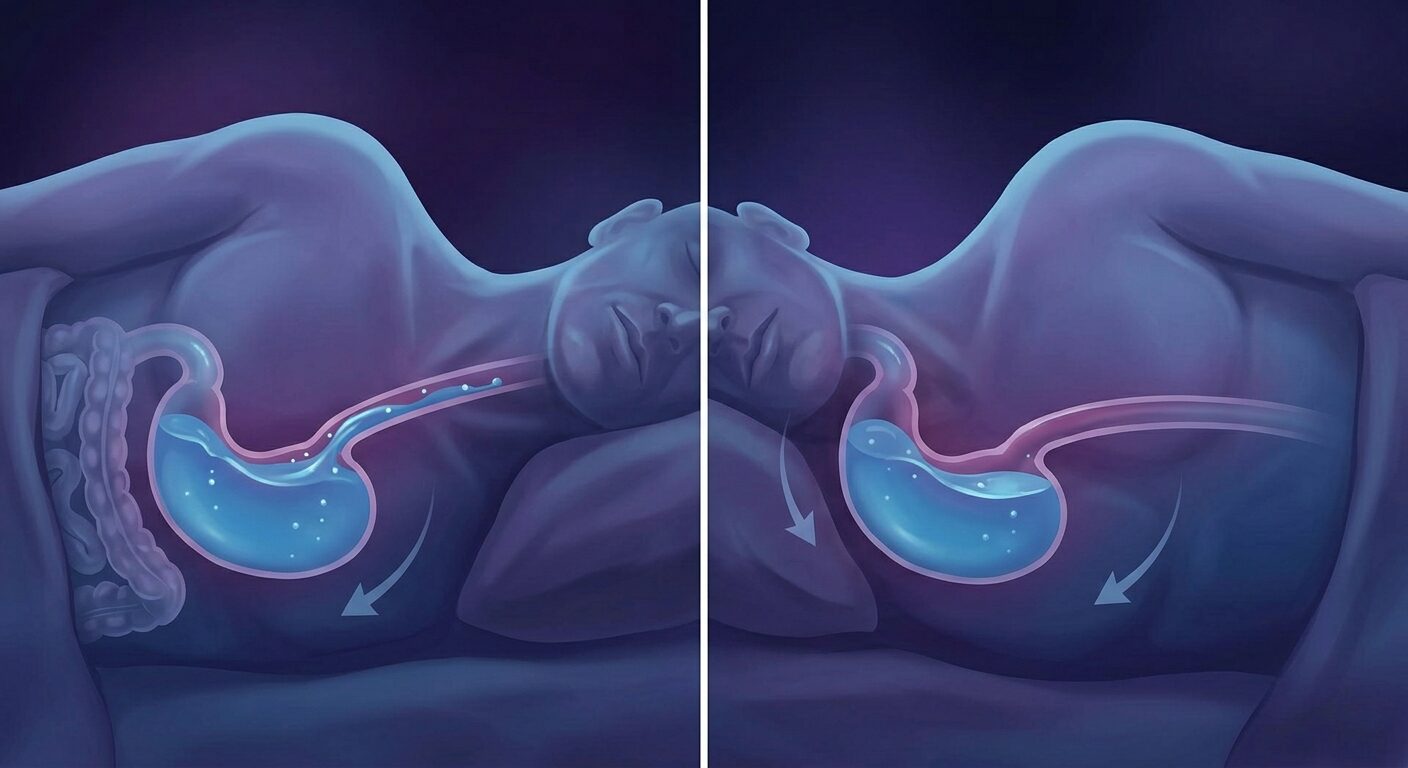
-
Sleep on the left side — positions the gastro-oesophageal junction above the acid pool, reducing reflux events significantly
-
Elevate the head of the bed 10–15 cm using bed risers or a wedge pillow (not extra pillows, which bend the neck without changing the angle of the oesophagus relative to the stomach)
-
Avoid sleeping on the right side or back if reflux is suspected — both positions increase acid exposure
Dietary Strategies
-
Stop eating at least 3 hours before lying down — a full stomach increases pressure that pushes acid upward
-
Reduce known triggers: alcohol (relaxes the sphincter), caffeine, spicy foods, citrus, tomato-based foods, and high-fat meals close to bedtime
-
Eat smaller evening meals — large volumes increase intra-abdominal pressure regardless of food type
-
Consider including alkaline foods (non-citrus fruits, vegetables, oats) at dinner to buffer acid production
Investigate the Root Cause
-
Test for H. pylori via urea breath test or stool antigen — the most common treatable cause of chronic reflux
-
Consider gastroscopy if symptoms are persistent, worsening, or accompanied by difficulty swallowing
-
Assess for low stomach acid (hypochlorhydria) — counterintuitively, insufficient acid can worsen reflux by impairing sphincter function and slowing gastric emptying
-
If currently on PPIs (proton pump inhibitors) long-term, discuss with your provider — long-term PPI use can worsen nutrient absorption problems that compound insomnia
This article is educational and not medical advice. Persistent reflux and sleep disruption warrant professional investigation, particularly to rule out H. pylori and structural causes.
When to Seek Professional Help
It’s time for professional investigation if:
-
Night waking coexists with morning throat irritation, hoarseness, or chronic cough that hasn’t responded to allergy treatment
-
Sleep disruption reliably worsens after eating late or drinking alcohol
-
Positional strategies (left-side sleeping, head elevation) help partially but don’t fully resolve the issue
-
You have digestive symptoms suggesting H. pylori or another gut infection
-
You’ve been investigated for insomnia, anxiety, or allergies without anyone assessing your oesophagus or testing for H. pylori
-
You’ve been on PPIs for more than 8 weeks without a clear plan for how long to continue
If you would like to see how we might be able to help you with this deeper, schedule a free consult here.
Frequently Asked Questions
Can acid reflux cause insomnia?
Yes. Nocturnal acid reflux — including silent reflux without heartburn — triggers vagal nerve irritation, micro-awakenings, and autonomic disruption during sleep. Studies using pH monitoring and polysomnography confirm that reflux events cluster in the 1–4 a.m. window and measurably fragment sleep architecture.
Can you have reflux without heartburn?
Yes. Laryngopharyngeal reflux (LPR) or “silent reflux” reaches the throat and airway without causing the classic chest burning of GERD. Symptoms include morning hoarseness, chronic cough, throat clearing, globus sensation, and unexplained sleep disruption — often misattributed to allergies or anxiety.
What is the best sleeping position for acid reflux?
Left-side sleeping. Research consistently shows it reduces oesophageal acid exposure by 70–80 percent because it positions the gastro-oesophageal junction above the stomach’s acid pool. Elevating the head of the bed 10–15 cm provides additional benefit.
Can H. pylori cause acid reflux and insomnia?
Yes. H. pylori alters gastric acid dynamics, damages the stomach lining, weakens the oesophageal sphincter, and creates chronic inflammation that disrupts cortisol, nutrients, and serotonin — causing reflux and insomnia through shared pathways. Treating H. pylori often resolves both.
Why does my reflux get worse at night?
Stomach acid production peaks in late evening and early morning, and lying flat removes gravity’s help in keeping acid below the sphincter. The combination of peak acid output and horizontal positioning makes nighttime the highest-risk period for reflux — and for sleep disruption caused by reflux.
When to Work With a Sleep Consultant
If silent reflux is fragmenting your sleep, the fix isn’t just elevating your pillow or avoiding spicy food. It’s finding out why acid is escaping in the first place — and that investigation often leads to H. pylori, low stomach acid, or gut dysfunction that’s been driving the problem quietly for months or years.
Riley Jarvis at The Sleep Consultant works with clients to uncover the root biological causes behind chronic sleep issues and build personalised protocols that address every layer — not just the symptoms.
Book a consultation at TheSleepConsultant.com.